Medically Reviewed by Dr Balraj Sandhu
Last updated on 12.06.2024
Measles- what causes it and why is it serious?
What is Measles?
Measles is a viral infection, that causes a distinctive rash and fever. It is highly contagious and can lead to serious complications including death. While it’s become much less common in Australia due to routine childhood vaccination, outbreaks still occur from time to time. Sometimes it is brought in to the country by non-immunised people, and it can also arise in communities where vaccination rates are low.
How is Measles spread? How do you get Measles?
Measles is highly contagious- it’s usually spread by the tiny droplets released when an infected person coughs or sneezes. These droplets are inhaled by another person, leading to infection. It can also be spread through direct contact, or by touching a surface that an infected person has contaminated.
It can take between 7 and 18 days after exposure to show signs of illness, though the typical incubation period is about 10 days. If an unvaccinated child is exposed to Measles, they have roughly a 90% chance of becoming ill themselves.
How long is Measles contagious for?
A person may be contagious with Measles for about 5 days before the start of the rash and for another 4-5 days after the rash first appears.
Who is most at risk of getting Measles?
Certain groups of people are more at risk of getting Measles:
- Children
- Pregnant women
- Babies under a year of age, who are too young to be vaccinated.
- People who have a weakened immune system due to medicines or serious illness.
- People born before 1966 tend to have natural immunity as Measles was common- people born after 1966 who have not had Measles or Measles vaccination are at a higher risk
What are the symptoms of Measles?
- At first it may seem like the common cold- with a runny nose, watery red eyes, a cough (which may be worse at night), fever and feeling tired.
- 2 to 3 days later a red rash appears, starting on the head and then involving the rest of the body over about 48 hours.
- The rash and the other viral symptoms generally continue for about a week, though the cough may continue for about 2 weeks.
- Sometimes secondary infections or complications may develop.
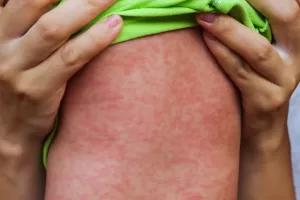
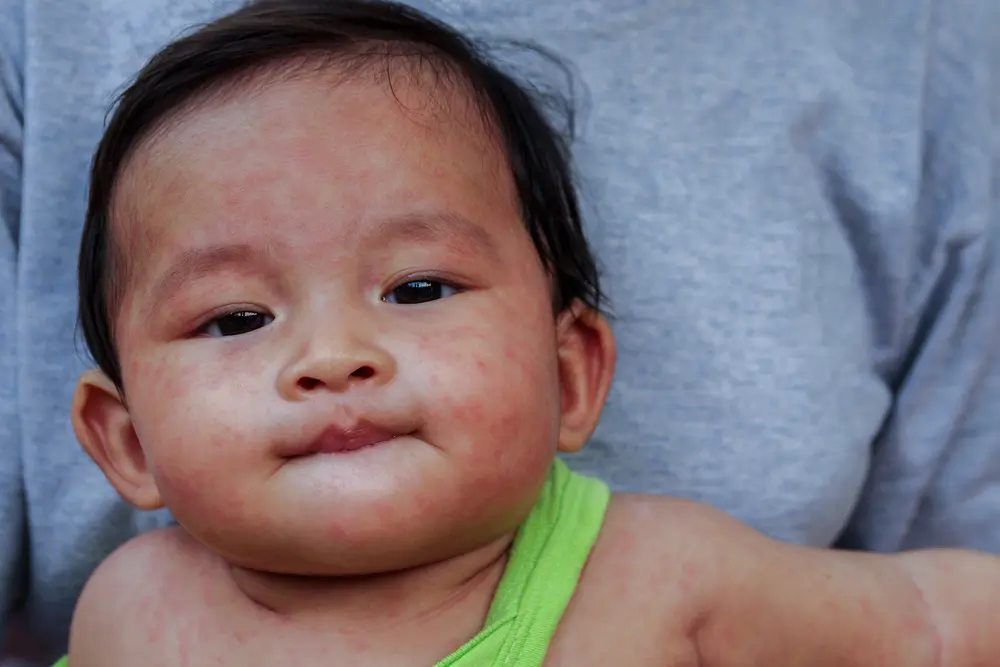
What does the Measles Rash look like?
Measles causes a distinctive dark red, slightly raised, blotchy rash. It tends to start on the head (often along the hairline and behind the ears) and progresses to the neck and the rest of the body. In the first couple of days there may also be spots in the mouth, on the inside of the cheeks- these are known as “Koplik spots” and have a whitish hue.
It is not an itchy rash.
What are the complications of Measles?
Complications can include:
- Ear infections
- Vomiting and diarrhoea
- Respiratory issues such as Croup, Laryngitis and Pneumonia
- Measles in pregnancy can lead to premature labour, miscarriage or stillbirth.
- Encephalitis (inflammation of the brain) and brain damage
- Liver infection( hepatitis)
- Blindness ( due to inflammation of the optic nerve)
- Subacute Sclerosing Panencephalitis (SSPE) is a rare degenerative brain condition that sets in many years after initial Measles infection (typically around 7 years later, though it can be longer). It occurs in 1 in every 100,000 cases of Measles. There is no cure for SSPE- it is a fatal condition.
Can you die from Measles?
Yes, deaths still occur from Measles, due to various complications, though pneumonia is the most common fatal complication. In Europe there have been 37 deaths so far in 2018.
How do you prevent Measles?
- The best way to prevent Measles is to get the MMR vaccine
- The MMR vaccine is offered to all children in Australia as part of the childhood vaccination schedule. It gives around 93% protection after one shot, and 97% after a second.
- It is generally very safe and effective.
- “Herd immunity” is important in protecting against Measles epidemics- this means that over 95% of kids need to be immunised to make the vaccine work for the entire community.
- There is an MMR vaccine at 12 months of age, and another at 18 months called MMRV (which also includes immunisation against chicken pox). A catch-up vaccine can be given at 4 years of age in children who didn’t get a second vaccine.
- People born after 1966 who have never had Measles or the MMR vaccine are also eligible.
- The MMR vaccine is often recommended for overseas travellers as well as healthcare workers or people working with children or the elderly.
- Booster vaccinations may be advised if there is an outbreak in a community.
- If a person has been exposed to Measles and has not been vaccinated, they may be given “Human normal immunoglobulin” or HNIG for short- this can help to reduce the risk of infection, if given within 6 days of exposure. It can be used in young babies, pregnant women or people with weakened immune systems (for example due to cancer, leukaemia or HIV)
Who shouldn’t have the MMR vaccine?
- Pregnant women (pregnancy should also be avoided in the month following MMR vaccine)
- People with significantly weakened immune systems- e.g. due to chemotherapy and certain illnesses such as HIV. A doctor can advise you if you’re not sure.
- People who have known allergies to ingredients in the vaccine
If you’re not sure, speak to your GP.
For how long should a person with Measles stay out of school or work?
- If a person has Measles, they should stay at home from work, school or childcare for at least 5 days after the Measles rash first appears.
- If an unvaccinated person or someone with a weakened immune system has been exposed to a known case of Measles they should be quarantined for 2 weeks after the exposure, to ensure they are not carrying it. This is because an infected person can spread Measles even before they develop the rash.
Can you get Measles twice?
If you’ve had Measles it’s rare to get it again. However, if a person’s immune system becomes weakened for some reason (such as serious illness or medication that affects the immune system), they may be at risk.
When should I see a doctor?
- If you think your child has Measles, it’s important to seek urgent medical advice to confirm the case.
- It’s a good idea to tell your GP or the emergency department of your concerns before you arrive for an appointment, so they can take precautions to prevent spread to other people(e.g. they may ask you to sit in a separate, quarantined waiting area).
Is there any treatment for Measles?
There is no specific treatment for Measles. It’s a virus, so antibiotics don’t work. General measures include plenty of fluids, rest and analgesia. Sometimes, if complications such as ear infections or pneumonia occur, antibiotics may be considered.
If you have concerns bout Measles you should speak to your doctor.
Renew a Specialist Referral Online
How to Renew a Specialist Referral Online If your specialist referral has expired, you may need to renew your specialist referral before your next appointment. This situation is common [...]
Do Specialist Referrals Expire? Referral Rules in Australia
Do Specialist Referrals Expire? Yes, in many cases specialist referrals in Australia expire after 12 months. However, the exact validity period depends on who wrote the referral and the type of referral. Understanding [...]
A Decade of Telehealth Medical Certificates- what we’ve learned.
A Decade of Telehealth Medical Certificates- what we've learned. For more than a decade, Qoctor has been providing medical certificates via telehealth to hundreds of thousands of Australians. During that time, the [...]