Anaphylaxis
Medically Reviewed by Dr Ali Zavery
Last updated on 13.06.2024
What is anaphylaxis?
Anaphylaxis is a severe life-threatening allergy. Normally, the immune system defends the body against threats such as bacteria and viruses. An allergy is when a person’s immune system reacts abnormally to something it’s exposed to- for example, certain types of food, pollen, animal dander, insect bites or medication. The immune system releases chemicals in response to the trigger.
In mild allergies, this can result in symptoms such as itchy eyes, hives and a runny nose. However, in anaphylaxis the allergic reaction is much more severe and can happen within moments of exposure to a trigger- a wave of chemicals is released by the immune system, quickly affecting a person’s breathing and circulation. It is a medical emergency and usually requires urgent treatment with an adrenaline injection.
How common is anaphylaxis?
In Australia, hospital attendances for anaphylaxis have increased for all age groups in the past 30 years. Food is the major cause of anaphylaxis in the 0-4 age group. There are around 170 known food types that can cause severe allergy.
- It’s thought that around 1 in 100 school children have anaphylaxis
- It’s more common in females than in males.
- Anaphylaxis causes 15 deaths per year in Australia.
- Death from anaphylaxis is rare, but almost always is preventable. Where anaphylaxis is triggered by a medication, death is more likely to occur.
What causes anaphylaxis?
- Following exposure to the trigger, there is a release of inflammatory substances from certain types of white blood cells, which are part of the body’s immune system
- These substances have a rapid effect on various parts of the body, including blood vessels, airways, the heart and the gut, leading to the typical symptoms of anaphylaxis.
Common anaphylaxis triggers include
- Foods such as peanuts, treenuts, fish, shellfish and others
- Medications- such as antibiotics, aspirin, intravenous contrast
- Insect stings and bites- from wasps, bees, fire ants, hornets, yellow jackets
- Latex
- Rarely, exercise is a cause of anaphylaxis- in some cases, exercise after eating certain foods or exercising in certain temperatures.
- A history of certain medical conditions increase the risk of having anaphylaxis, including the presence of allergies, asthma.
What are the symptoms of anaphylaxis?
Symptoms & signs of anaphylaxis include
- Tight or constricted breathing
- Swelling of the tongue
- Difficulty speaking and sometimes a hoarse voice
- Swelling or tightness in the throat
- Rapid heart rate and low blood pressure
- Loss of consciousness/collapse
- Pale appearance and floppiness in small children or babies
Sometimes there may be milder signs of allergy before the above symptoms start, which can include:
- A tingling sensation around the lips or mouth.
- Hives or welts
- Abdominal pain and vomiting (although these are viewed as signs of anaphylaxis in the case of insect allergy)
In around 1 in 5 cases, there may be a second bout of anaphylaxis within 12 hours of the first. This is called biphasic anaphylaxis.
Why is anaphylaxis becoming more common?
It’s not certain why anaphylaxis is on the rise, but there are a few theories:
- Reduced exposure to germs and infections in early childhood (due to more sanitised living conditions) could lead to a higher risk of allergy. This is sometimes referred to as the “hygiene hypothesis”. Research has shown that children from bigger families, as well as those who have close contact with pets or farm animals are less likely to get allergies and anaphylaxis, which may support this theory.
- Delayed exposure to allergenic foods such as nuts and eggs, until later in childhood could be a factor.
- Theories have been put forward that taking antibiotics may affect the natural bacteria in the bowel, and that this could have an impact on the immune system.
- Some studies have shown that the further a population lives from the equator, the higher the risk of allergies. This may be due to differences in Vitamin D levels (we get most of our Vitamin D from sun exposure).
- Different ways of preparing food may be relevant. For example, it appears that roasting peanuts can make them more likely to cause allergy, whereas boiling them reduces the risk. Variations in food preparation may in part explain differences in allergy rates between different countries.

Do complementary or alternative tests for allergies work?
- There are many types of alternative therapies that claim to be able to diagnose allergies, but these lack evidence and are best avoided.
- Methods which lack evidence include kinesiology, vega testing, hair analysis, cytotoxic food testing, iridology, reflexology, Alcat testing, IgG food allergy testing and Rinkel’s intradermal testing.
How is anaphylaxis diagnosed and treated?
- A medical history, examination and allergy tests (bloods and/or skin prick testing) will usually be performed.
- If you’ve had an episode of anaphylaxis (or a suspected episode) your GP will usually refer you to an immunology or allergy specialist for assessment and advice.
- You’ll need education on how to avoid your trigger- a dietitian specialising in allergies may be helpful if it’s a food trigger.
- It’s advisable to wear a medical alert bracelet or necklace, stating that you have anaphylaxis, and the triggers involved
- An ASCIA action plan is usually required for children in childcare or school, but is advisable for anyone with a history of anaphylaxis.
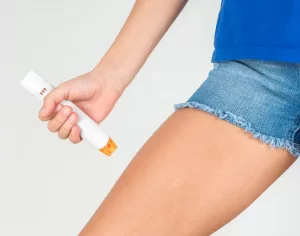
- An adrenaline (epinephrine) autoinjector is usually prescribed- it’s important to be advised about how and when to use this. If the auto-injector is used, it’s also essential to call an ambulance immediately.
- Over time, some allergies may decrease. For example, 20% of children grow out of peanut allergies. Ongoing follow up with an allergy specialist means re-testing can be arranged at appropriate intervals.
- Desensitisation therapy (immunotherapy) can be effective in some cases and may be recommended by an allergy specialist.
For more information on allergies and anaphylaxis, speak to your doctor or check out the ASCIA website.
Resources:
https://allergyfacts.org.au/allergy-anaphylaxis/food-allergy
Renew a Specialist Referral Online
How to Renew a Specialist Referral Online If your specialist referral has expired, you may need to renew your specialist referral before your next appointment. This situation is common [...]
Do Specialist Referrals Expire? Referral Rules in Australia
Do Specialist Referrals Expire? Yes, in many cases specialist referrals in Australia expire after 12 months. However, the exact validity period depends on who wrote the referral and the type of referral. Understanding [...]
A Decade of Telehealth Medical Certificates- what we’ve learned.
A Decade of Telehealth Medical Certificates- what we've learned. For more than a decade, Qoctor has been providing medical certificates via telehealth to hundreds of thousands of Australians. During that time, the [...]